Introduction: The Hemophilia Challenge in IndiaHemophilia, a rare genetic disorder characterized by the body's inability to form stable blood clots, presents a significant public health challenge in India. With a population exceeding 1.4 billion, the nation is estimated to have a staggering 1 to 1.5 lakh cases, yet a vast majority—nearly 80%—remain officially undiagnosed. While prophylaxis, a preventive treatment, is recognized globally as the gold standard for managing the disease and preventing long-term disability, its adoption in India is critically low. This case study analyzes the profound socio-economic impact of this disparity, explores the systemic barriers to effective care, and outlines a strategic, multi-pronged "way forward" to align India's hemophilia care with international best practices.
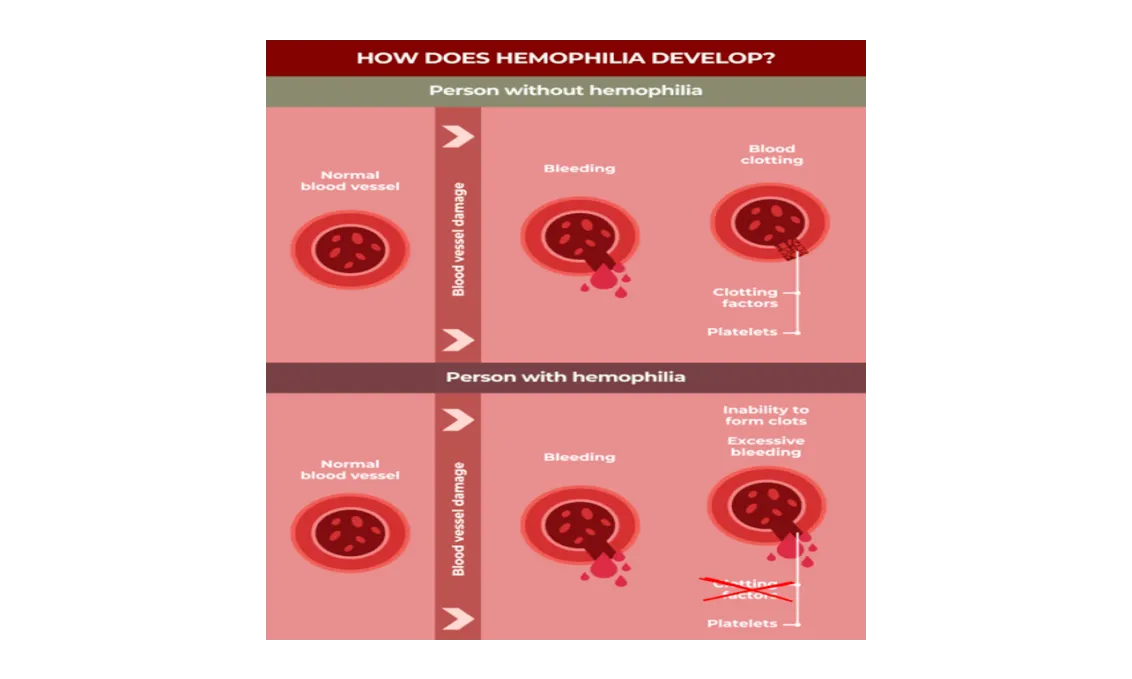
/*The Silent Crisis: The Burden of Hemophilia*/
/*Hemophilia*/ is a debilitating genetic disorder that severely impacts a patient's life by preventing blood from clotting properly due to a lack of specific clotting factors, typically /*Factor VIII*/. The consequences extend far beyond simple bleeding, as even minor injuries can lead to severe, spontaneous internal bleeding into joints and muscles. If left untreated, these repeated bleeds cause irreversible joint damage, chronic pain, and permanent disability. In India, this condition creates a cycle of despair, with chronic bleeds often leading to school dropouts, unemployment, and a significant loss of productivity, which in turn perpetuates social exclusion and economic hardship for both the patient and their family.

/*Prophylaxis: The Gold Standard in Practice*/
/*The gold standard for managing this condition is prophylaxis, a paradigm shift from reactive to proactive care. */Unlike traditional "on-demand" therapy, which treats bleeds as they occur, prophylaxis involves the regular, preventative infusion of the missing clotting factor, even when there is no active bleeding. This strategy aims to keep clotting factor levels stable, thus preventing bleeds from happening in the first place and protecting the joints from irreversible damage. In developed countries, where roughly 90% of patients use this treatment regularly, prophylaxis has been proven to enable a near-normal life expectancy and a dramatically reduced disability rate.
/*Navigating the Disparity: A Socio-Economic Analysis*/
Despite its proven efficacy, a significant gap exists between global and Indian contexts. While developed nations have strong policy support and high access rates, most patients in India still rely on outdated on-demand treatment. This disparity is a direct result of several key barriers: a profound lack of awareness among families and local doctors, limited diagnostic infrastructure, particularly in rural and small towns, and substantial socio-economic obstacles such as the high cost of tests and treatment. Furthermore, social stigma surrounding the disease can deter families from seeking a diagnosis or long-term care, making a challenging situation even more dire.
/*The Path Forward: A Multi-Pronged Strategy*/
/*To close this critical gap, a strategic and coordinated effort is essential, requiring a multi-pronged "way forward*/." Key initiatives must include integrating hemophilia treatment under national health schemes like Ayushman Bharat to provide subsidized clotting factors, thereby overcoming economic barriers. Simultaneously, nationwide public awareness campaigns and training programs for primary healthcare providers are necessary to facilitate early diagnosis and dismantle social stigma. Finally, promoting indigenous manufacturing of clotting factors and encouraging research into newer technologies like non-factor drugs and gene therapy will ensure a sustainable and more patient-friendly future for hemophilia care in India.
/*Conclusion: A Case for Change*/
The implementation of this comprehensive strategy is not just a medical aspiration; it is a socio-economic imperative. Consider the case of a young boy with hemophilia. In the current system, his life is defined by constant pain, missed school days, and the looming threat of permanent disability. With the proposed "way forward," however, he could receive regular prophylaxis, allowing him to attend school, play with his friends, and grow into a productive member of society. This shift from reactive, expensive care to proactive, preventative treatment offers not just improved health outcomes but a path to a life of dignity, proving that systemic change can fundamentally transform the lives of hemophilia patients across India.